Some of you have heard that we recently got very bad news about our son, Adrian. He was diagnosed with acute lymphoblastic leukemia on June 25.
Since it’s been chaotic for us over the last few weeks, we have not had time to notify all of our friends nor give many updates. We’ve set up this blog to provide (hopefully) semi-regular updates and some information about leukemia for those of you that are interested in tracking the progression of treatment.
This first post is a lot longer (and much more detailed) than what we’ll normally post, because here we’ll get you caught up from the beginning to current.
Feel free to ping us with questions and/or leave comments.
Initial signs/ hospital admission (June 8-23)
Monday, June 8, started as a normal morning. Sarah dropped off AJ at preschool that day and then went to work. AJ seemed excited about school that day and was not acting sick. Mid-morning we got a call from his teacher, Miss Shannen, saying that AJ was not feeling well. He did not feel like participating in any of the morning activities and had been lying on the couch. She asked if we could pick him up. We called our nanny to pick him up, and in the meantime we found out that he had a fever of 101°. By the time we got him home, his fever was 103°. This seemed high to us, so Sarah took him to the pediatrician’s office that afternoon. The doctor said his fever was probably caused by a virus, but he also had an ear infection so we were prescribed antibiotics.
Over the next several days, the fever went away and AJ’s ears seemed to get better. By the weekend, he was back to normal. We had several outings, played in our little swimming pool and went to some friend’s house for dinner where he played with other kids. All seemed fine. On Monday he went back to preschool as usual.
On Wednesday June 17, something strange happened. AJ developed a rash all over his body. During the visit to the pediatrician the week prior, the doctor had told Sarah that the virus causing his fever might be roseola and that a rash could develop after the fever went away. We looked up roseola online and his rash looked consistent with a roseola rash, so we weren’t too worried. As the rash started to go away over the next couple days, however, he began to run another low-grade fever which seemed odd. Why would the fever come back?
Grandma and Grandpa Utter came to visit that weekend. AJ’s fever remained low grade through Saturday but he became more and more lethargic. He skipped soccer on Saturday. On Sunday, Sarah had to leave to NYC for a business trip. We discussed getting AJ back into the pediatrician’s office on Monday morning if the fever was not gone by then.
On Sunday night, AJ’s fever spiked to around 104, and with Grandma and Grandpa’s help, we took it down with Tylenol, Ibuprofen, and sponging him down.
Brian called Sand Point Pediatrics on Monday and got AJ back in for an appointment that afternoon. At the doctor, AJ’s fever had dropped a bit, and he was told that the second fever was likely not related to the first, and probably just bad luck. AJ would get better over the next couple of days.
But at home that afternoon, he seemed to get worse. His fever spiked back up and he started complaining about his ears again. Despite pushing liquids, he also seemed really dehydrated and his mouth was super dry. We thought it might indicate a new bacterial infection in his sinuses or throat in addition to his ears. He also looked pale.
Brian gave AJ more sponge baths that night, and Tylenol and Ibuprofen, as he got up to around 104-105 degrees. We were worried at this point.
The next morning, Tuesday June 23, Brian called back in to get another appointment at Sand Point Pediatrics to take a look at his ears, sinuses, and talk about the fever. We were assigned to a different doctor for this trip, and got in at 2:15pm.
It was a pretty short visit. Dr. Nyweide looked at his ears and mouth, and examined his belly, which she noted looked swollen. Nothing good was happening, and the doctor bluntly told Brian she was concerned about him and asked him to take him over to Children’s Hospital immediately for blood work. She was pretty non-specific about what might be wrong, and Brian was really alarmed.
After getting the blood work done, we were told we’d have results within a couple hours. Brian was at home at around 4pm, sitting in the bed with AJ, texting Sarah in NYC, when he got the call from Dr. Nyweide with the bad news. She told him the blood work came back irregular and it looked like leukemia or lymphoma. We needed to get back to the hospital immediately.
That first night is still pretty blurry and was very difficult. Brian first called Sarah in NYC, which was miserable for both of us. She called the airline to get on an earlier flight back to Seattle. He then called our close friend Beckie Brocies and asked her to come over to relieve our nanny Carather to take care of AJ’s sister Camille. Brian then called his parents and gave them the bad news. Sarah called her Mom and sister to let them know what was going on.
We were admitted through the ER at Children’s. Our close friend Diana Olson had heard through Brian’s parents and she came by to be with AJ and Brian. We spent about four hours in the ER getting tests (x-rays, exams, blood work) and an IV put in AJ’s hand.
Later that night we were brought up to the 3rd floor Hematology/Oncology ward. It was hard for AJ to sleep in a strange bed with nurses coming in every hour or so to check on him. Brian didn’t sleep.
At the Hospital (June 23-July 4)
Sarah got back into town the next morning and came straight to the hospital. Grandma and Grandpa Utter had returned to Seattle the night before as soon as they heard the news. We had a very sick boy on our hands. The next day and a half was spent getting AJ’s blood counts up so that he could be in a condition stable enough to withstand the procedures that would confirm a diagnosis. For those interested in the numbers, here is a summary of what his counts looked like:
- HCT (hematocrit): this is the measurement of red blood cells, which carry oxygen through the body. Normal range for a child AJ’s age is 31-48%. AJ was a 12% when admitted to the hospital, which is severely anemic. This was why he was lethargic and looked so pale. We needed to get him up to at least 20% through blood transfusions. He required 6 blood transfusions. Each transfusion occurred slowly over several hours in order to not put too much stress on his heart and to watch for allergic reactions. It was amazing to see the color return to his face and body as his red blood cell count went up.
- Platelets: these are the cells that make the blood clot. Normal range is 150K – 500K. AJ was at 63K when admitted to the hospital but dropped to as low as 11K. He needed to be at least 20K before undergoing the diagnostic procedures which required anesthesia. He required a platelet infusion in order to get his count up.
- White blood cells: these are cells that fight infection. Normal levels are between 5K and 12K, but AJ’s count was low at 1.2K. Having a really high white blood cell count is actually worse than having a really low one when you have leukemia (and if you are above 50K, then it worsens your prognosis).
- ANC (absolute neutrophil count): Neutrophils are a type of white blood cell. The ANC is a good measurement of how your immune system is functioning, and in fact we pay more attention to this number than the white blood cell number. Normal range is above 1000 (and can go up to 5000 or more). At below 500, you must avoid crowds, school and social events. At below 200, you are severely immune suppressed, need to avoid public places and likely need to be on antibiotics. AJ’s ANC was at 0 when we were admitted to the hospital.
On Thursday, June 25, AJ’s blood counts were stable enough for him to undergo a bone marrow aspiration and a lumbar puncture (spinal tap), which required him to be sedated. Holding him as he “went to sleep” in the operating room was one of the most difficult things we’ve had to do as parents. These two tests would enable the doctors to properly diagnose AJ.
Later that afternoon, Dr. Kutny, the Hemotology-Oncology fellow, gave us the official diagnosis. AJ did in fact have leukemia. It was ALL (acute lymphoblastic leukemia) and the subtype was pre-B.
What is leukemia?
Leukemia is cancer of the blood-forming tissue known as bone marrow. Bone marrow produces blood cells. With leukemia, the bone marrow creates an overabundance of abnormal young white cells known as “blasts.” These blasts do not function as they should and the bone marrow becomes packed with them, literally crowding out the other normal cells (red, white, platelets). That is why normal cell counts are so low, and the overcrowding is why many people have bone pain as an initial sign of leukemia.
Who gets childhood leukemia and what causes it?
Acute leukemia is the most common childhood cancer. That said, it is very rare, with approximately 3500 children in the US diagnosed each year. It seems to strike children randomly, but is most commonly diagnosed at ages 2 to 7, more common in Caucasians than other races and slightly more common in boys than girls. The cause is unknown. Since there are many different types of leukemia, scientists believe that each type may have different causes. In general, it is believed that genetic mutation, environmental factors and potentially viral factors may all contribute to leukemia. Before being diagnosed, AJ had never had any health issues at all.
After hearing about AJ’s diagnosis, many people have asked us what the signs and symptoms of leukemia are, so we are listing them below (though keep in mind leukemia is very rare and many of the symptoms mimic those that are normally associated with minor illnesses such as the flu):
• Fatigue or weakness
• Pale skin
• Unexplained or prolonged fever
• Loss of appetite
• Irritability
• Bone pain
• Bruising or unusual bleeding (bleeding gums, nosebleeds)
• Enlarged liver, spleen or lymph nodes
In hindsight, AJ had many of the signs including fatigue, bruising (he tended to bruise easier than his sister), and pale skin. It was the prolonged fever that was the biggest red flag for us.
What is AJ’s prognosis?
Once we knew AJ had leukemia, all of the news we have had since then about his prognosis has been positive. For one, he was diagnosed with ALL which has a better prognosis than other types of leukemia (such as AML, CML, JMML). Treatment of childhood ALL is one of the success stories of medicine in recent decades. In the 1960s, patients with ALL died within a few weeks or months. Cure rates rose to 40% in the 1980s, and are up to 80-85% today.
AJ has several other factors that improve his prognosis:
- Cell type. AJ has the ALL sub-type of Pre-B, which has a better prognosis than other sub-types.
- His age (4). Children between the ages 2-9 typically fare better than infants or older children.
- White blood count at diagnosis. AJ had a WBC of <50K, which has a better prognosis than a WBC >50K.
- Cytogenetic results. Some patients have certain chromosomal characteristics in their leukemia cells which impact prognosis. AJ happens to have what’s called the TEL-AML1 fusion, which is where the TEL gene on chromosome 12 moves to the AML gene on chromosome 21. Children with this fusion tend to have very good outcomes.
- Response to treatment. AJ saw a rapid reduction of blasts once he started treatment, with his blast count dropping to 0 within a few days. A bone marrow aspiration on day 14 of treatment confirmed no leukemia cells and AJ was designated an “early rapid responder” which is another favorable factor in prognosis.
Given the above factors, we believe AJ has a 90% or higher chance of being cured.
What is the treatment?
AJ’s treatment will be pure chemotherapy. At this point, assuming he continues on the track he is on, neither radiation nor bone marrow transplant will be needed. His treatment is divided into several phases, with the most intense chemotherapy in the first 6 months, and a less intense maintenance period that lasts 3 years (boys require maintenance that lasts one year longer than girls). The phases are as follows:
- Induction: this is 4 weeks of intense chemotherapy via combination of IV, injection, pills and spinal taps. The goal is to come out of this phase in remission. Various drugs are given to target fast-growing cells, including the steroid dexamethasone (which is the drug we are seeing the most side-effects from – moodiness, drastic increase in appetetite, swollen face and belly).
- Consolidation: another 4 weeks of chemotherapy with a different mix of drugs, but blood counts are allowed to recover. Treatment is on an outpatient basis.
- Interim maintenance: 8 weeks of chemotherapy with a different mix of drugs.
- Delayed intensification: 8 weeks of intense chemotherapy, combination of IV, injection, pills and spinal taps.
- Maintenance: 3 years. Less intense drugs given in 12 week cycles to prevent recurrence.
Finally sent home (July 4-July 12)
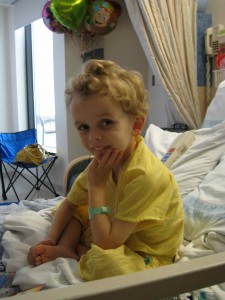
AJ at the hospital before release.
Once AJ was diagnosed with ALL, he began chemotherapy the next day, on June 26. He had surgery to insert a central line (called a port-a-cath or port) into his chest. The port allows for easy and fast administration of chemotherapy and also reduces the need for “pokes” as blood draws can be taken directly from the port.
At that point he was still fighting a respiratory infection as well as double ear infections, in addition to a continued fever. Getting rid of the infections and fever was the priority. He was on a wide spectrum of antibiotics and also had to have both ear drums punctured while he was sedated. After about another week of being in the hospital, on the evening July 4, we were discharged. However, we had to be trained on how to administer IV antibiotics as we had to continue giving him antibiotics through his port for 3 days after we got home.
Once home, AJ began to do really well. He had lost about 9 lbs in the hospital (he went from 38 lbs down to 29 lbs – so it was a huge percentage of his body weight). The steroids kicked in and he has been eating non-stop. He is eating an impressive amount of food. A typical breakfast includes 2 scrambled eggs, several pieces of toast, a yogurt, 5 or 6 mini pizzas, 3 or 4 fish sticks, some fruit, chips and salsa, crackers, cheese and 3 glasses of milk. And yes, that is just breakfast. He is usually hungry for lunch 2 hours later and is constantly snacking between. Needless to say, he is gaining the weight back. He has become food-obsessed and likes to plan what he is going to eat several meals ahead. This is an expected part of the induction phase because he is on steroids. For parents of a child who normally eats like a bird, it is disconcerting, but the steroids play a big role in killing the leukemia cells and preventing their return. After the first phase of treatment, the steroid use becomes a lesser part of the chemotherapy.
Other than eating, he is starting to gain back some of his energy and we are starting to see some of his blood counts improve. The first week out of the hospital we had to take him back to the Hemotology-Oncology clinic at Children’s every other day for blood draws and check-ups with the doctor. This will become less frequent as his counts go up.
We’ve had to take extra precaution when it comes to germs at home. Frequent hand washing and sanitizing is a must, and we are trying to keep the home environment as clean as possible in order to avoid any type of infection since AJ’s immune system is so weak. We also need to screen visitors as no one that has been sick or around someone sick should be exposed to him. The biggest thing we need to monitor is fever. We need to check AJ’s temperature multiple times a day, and at the first sign of fever we need to call the hospital. We have been told that we should expect that he may need to be readmitted to the hospital on occasion during treatment.
We have withdrawn AJ from preschool, but plan to have him re-enter after 6 months. His sister Camille does not need to limit her activities, although we have to be careful who she plays with and make sure that she washes her hands immediately after going out in public.
On Friday, we got the news that AJ is an “early rapid responder” to treatment (discussed in the prognosis section earlier) which was a great way to start the weekend. His most recent blood counts from Friday are below.
HCT (red blood cells): 29%
Platelets: 93K
White blood cells: 3.4K
ANC: 884 (yeah! Finally above 500 ☺)
These counts have all improved dramatically. We are cautiously optimistic that we will continue to see improvement. While AJ has a long, tough road ahead of him, we believe he is a very strong boy who will get through this. Please continue to keep him in your thoughts and prayers.
We are grateful to all of our friends and family that have helped us to date. Thanks to all of you for the visits, cards, gifts, meals and babysitting/entertaining AJ’s little sister Camille. And thanks to all of you that have offered help – we may be taking you up on your offers, though we have had great coverage and support to date. Brian’s parents spent the first 2 weeks with us, and Brian’s sister Heather flew out for the first few days after AJ was admitted to the hospital. Brian’s parents were followed by Sarah’s mom and her husband Larry. Then Sarah’s sister Laura arrived, and she is still here helping out. In addition, our nanny has been very supportive. Overall we have been very fortunate and appreciate all the help.
19 Comments